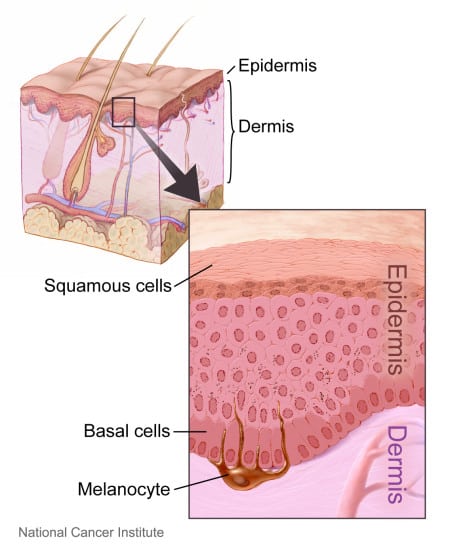
Basal cell carcinoma (BCC) is a form of skin cancer that develops in the top layer of the skin. It is by far the most common type of skin cancer—of the 3.5 million cases of skin cancer diagnosed every year in the United States, nearly 80% are basal cell carcinomas.
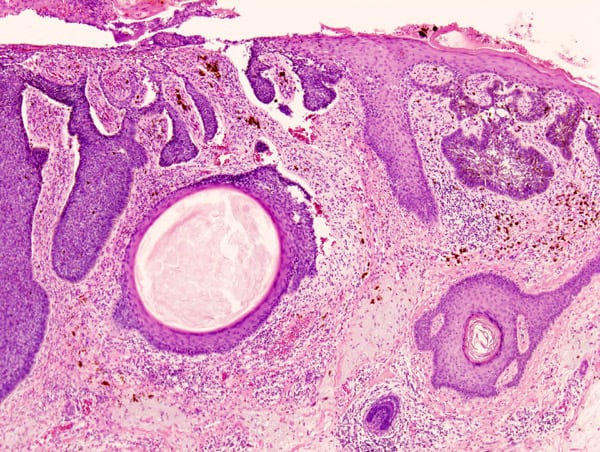
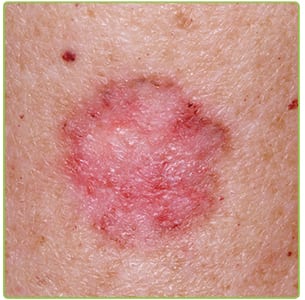
BCCs are cancerous lesions or tumors that are made up of damaged or mutated basal cells. These tumors form in the outer layer of the skin, and appear as small bumps or sores. BCCs rarely spread beyond the original location of the cancer.
Like all forms of cancer, basal cell carcinomas are the result of damage to the DNA of the cell. When a cell is damaged in certain ways, its DNA mutates, which can cause healthy cells to turn cancerous. This unregulated cell growth causes the formation of cancerous lesions or tumors.
While BCCs may form anywhere on the body, the most often appear on areas that are regularly exposed to the sun, such as the arms, neck, and face.