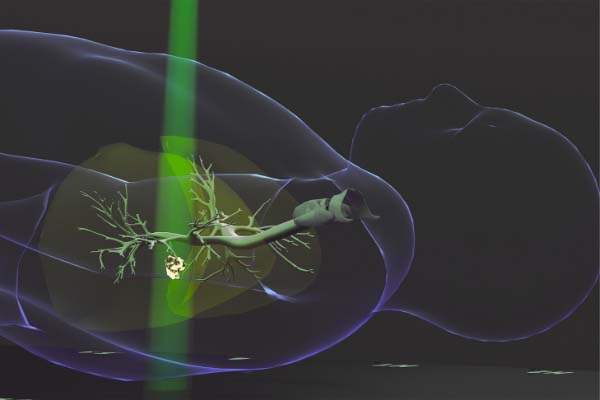
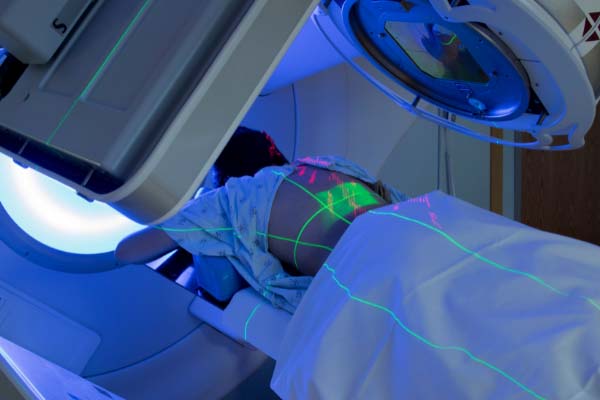
Radiation therapy is a common, effective, and painless cancer treatment. It can be used as a standalone treatment or can be part of a comprehensive plan that includes surgery or chemotherapy. Radiation therapy is used to kill cancer cells with concentrated X-ray beams.
If you or a loved one has recently received a cancer diagnosis, there is a good chance that radiation therapy will be a part of the treatment plan. With that in mind, the Charlotte area cancer treatment team at SERO wants to ensure that our patients and their families have access to the information that they need.
Below, we answer common questions about radiation therapy so that you and your loved ones can have peace of mind when you begin this journey.