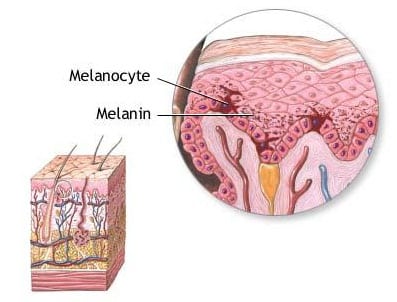
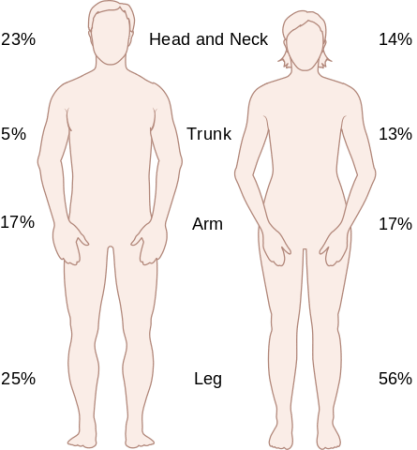
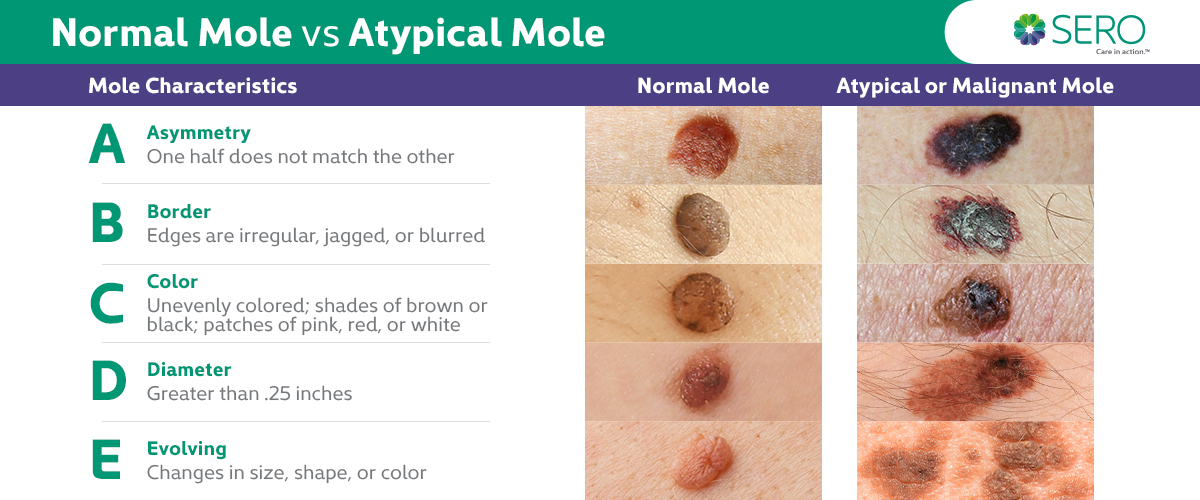
Melanoma skin cancer is the most serious form of skin cancer that occurs when pigment-producing cells (melanocytes) grow out of control. This aggressive form of skin cancer can develop anywhere on the body, but most commonly appears in areas exposed to the sun, such as the face, neck, chest, back, shoulders, and legs. While asking “what is melanoma?” is common, understanding its characteristics is crucial for early detection. For comprehensive information, download our free Skin Cancer eBook.
While melanoma is the least common type of skin cancer, accounting for only 2% of all skin cancer cases, it is also the most serious and dangerous.
In this article, we’ll discuss what melanoma is, how to recognize it, and steps you should take if you think you might have this type of skin cancer.